
Your Heart Is Not a Metronome: The Science of Heart Rate Variability
If you check your pulse and count 60 beats per minute, it is natural to assume your heart is beating exactly once every second. This assumption—that a healthy heart beats with the steady precision of a metronome—is incorrect. In a healthy body, the time interval between each heartbeat changes constantly.
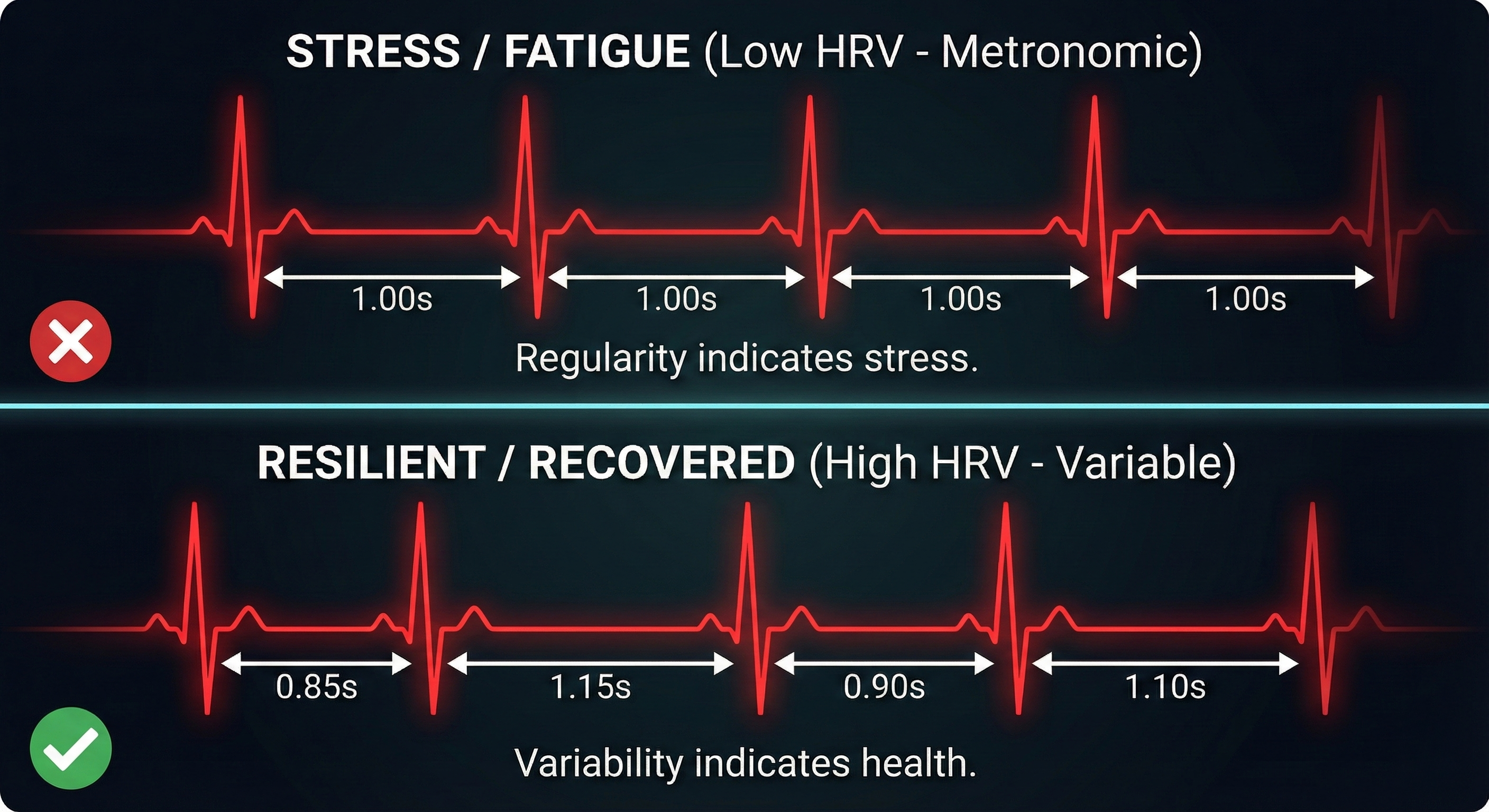
One beat might happen 0.85 seconds after the last, and the next might happen 1.15 seconds later. This fluctuation is called Heart Rate Variability (HRV). This article explains the physiological mechanisms behind HRV without oversimplification. By the end of this post, you will understand:
- Why a "consistent" heart rate is actually a sign of stress.
- The link between your nervous system and your heart rhythm.
- Why your heart rate changes when you breathe (Respiratory Sinus Arrhythmia).
- How to use HRV data to optimize your health and fitness.
What is HRV?
Heart Rate Variability is the measurement of the time difference between consecutive heartbeats. Scientists call these "inter-beat intervals" or R-R intervals (named after the "R" spike seen on an ECG graph). While your Heart Rate counts the total number of beats in a minute, HRV measures the irregularity in the timing of those beats.
- Low HRV: The time between beats is very consistent (e.g., almost exactly 1 second every time). This usually indicates the body is under stress, fighting an illness, or fatigued.
- High HRV: The time between beats fluctuates significantly. This generally indicates that the body is recovered, resilient, and ready to handle stress.
The Physiology: The Autonomic Nervous System
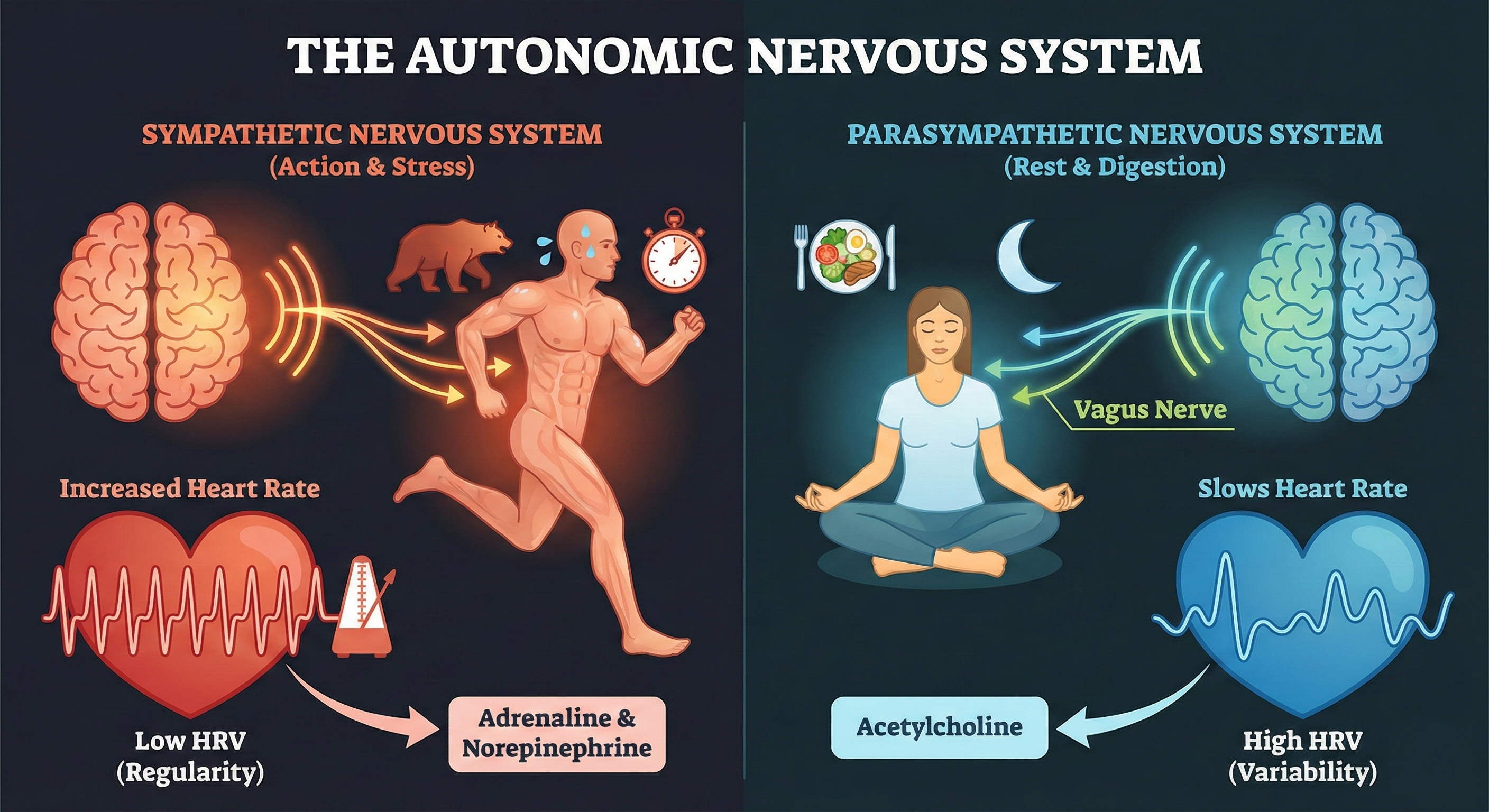
HRV acts as a window into your Autonomic Nervous System (ANS). This is the part of your nervous system that regulates involuntary functions like digestion, blood pressure, and breathing. The ANS consists of two major branches that influence the heart in opposite ways:
-
The Sympathetic Nervous System This system mobilizes the body for action. It is dominant during exercise, stress, or perceived danger. When active, it releases norepinephrine, which accelerates the heart rate and makes the rhythm more regular (lowering HRV).
-
The Parasympathetic Nervous System This system manages "rest and digestion." It is dominant during sleep and relaxation. Its primary connection to the heart is the Vagus Nerve. When active, the Vagus nerve releases acetylcholine, which slows the heart rate. Crucially, the Vagus nerve acts rapidly—it can slow the heart down in a fraction of a second. This rapid modulation causes the time between beats to vary, resulting in High HRV.
Key Takeaway: HRV is not random. It is the result of these two systems competing. A high HRV means your Parasympathetic system is active and responsive, capable of slowing the heart down quickly when needed.
The Link Between Breathing and Heart Rate
One of the main drivers of HRV is your breathing. You can test this right now: feel your pulse and take a slow, deep breath. You may notice your heart rate speeds up as you inhale and slows down as you exhale.
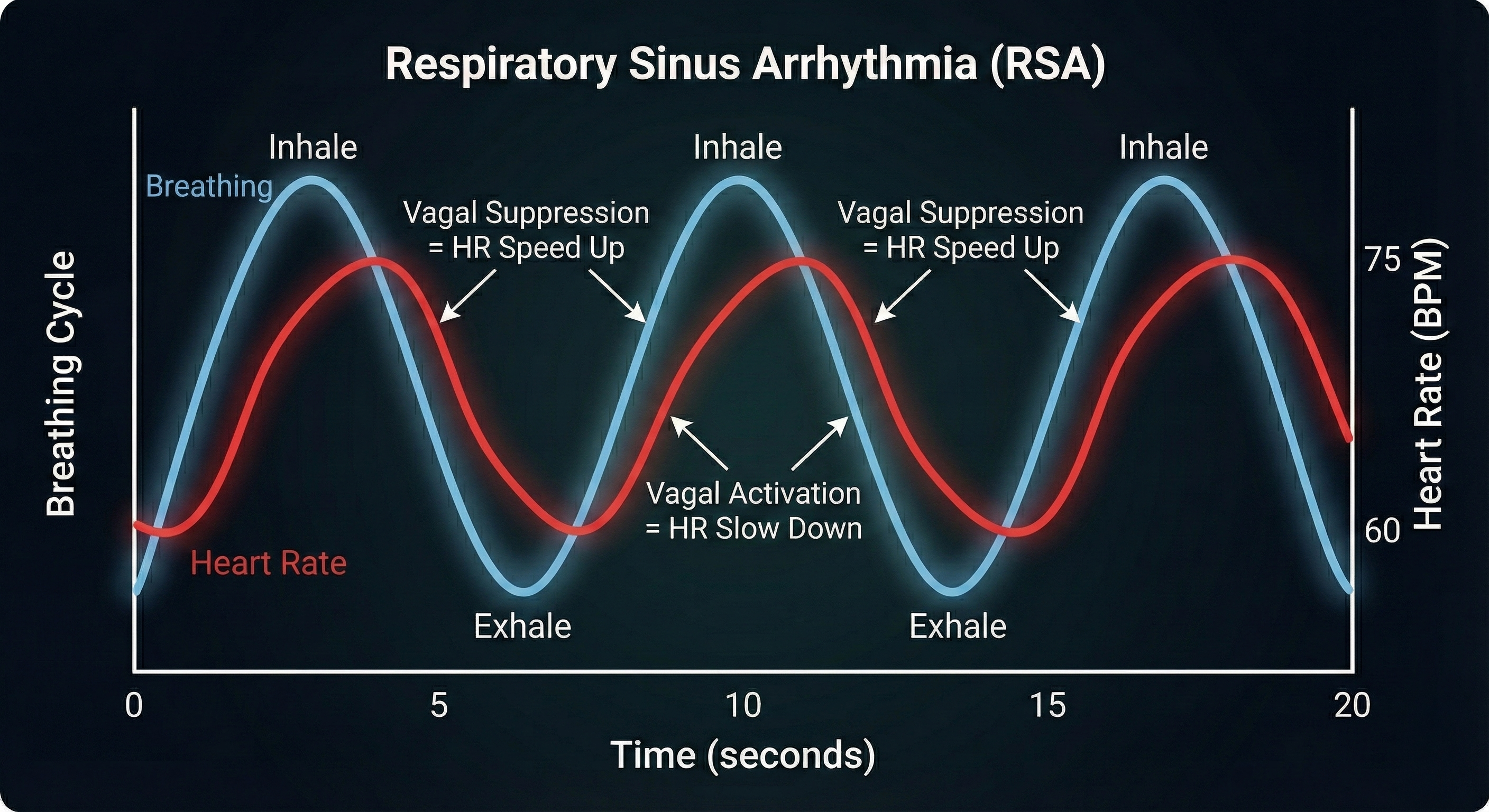
This phenomenon is called Respiratory Sinus Arrhythmia (RSA).
- Inhalation: The Vagus nerve is temporarily suppressed, allowing the heart rate to rise.
- Exhalation: The Vagus nerve becomes active again, rapidly slowing the heart rate.
This cycle creates a wave-like pattern in your heart rate. Because this variation is driven by the Vagus nerve, RSA is a direct measure of your parasympathetic (rest and recovery) status.
Measuring HRV: The "Gold Standard" Metric
If you look at raw HRV data, it is just a list of milliseconds (e.g., 800ms, 850ms, 790ms). To make this useful, apps and scientists use a mathematical calculation called RMSSD (Root Mean Square of Successive Differences).
We use RMSSD because it focuses specifically on the differences between adjacent beats. This filters out slower, long-term trends and isolates the rapid changes caused by the Vagus nerve. Therefore, RMSSD is the most accurate metric for tracking daily recovery and parasympathetic activity.
Note: You can find the mathematical formula and a step-by-step calculation example in the Appendix below.
How to Measure HRV Correctly
For HRV data to be useful, consistency in measurement is critical. Random or inconsistent measurements will produce unreliable data that cannot guide training or recovery decisions.
Measurement Protocol
Follow these guidelines for accurate, comparable readings:
-
Time of Day: Measure first thing in the morning, before getting out of bed, checking your phone, or drinking coffee. Your body is in a similar state each morning, making comparisons valid.
-
Body Position: Use the same position every day—either lying down or sitting upright. Do not switch between positions, as this affects HRV values.
-
Duration: Most apps require 2-5 minutes of data. Stay still, breathe normally, and avoid talking or moving.
-
Consistency: Measure at the same time, in the same position, every single day. Missing measurements creates gaps in your baseline data.
What Devices Can Measure HRV
Not all devices are created equal. Accuracy varies significantly:
High Accuracy (Medical-Grade):
- Chest strap heart rate monitors
- ECG-based wearables
Moderate Accuracy:
- Wrist-based optical sensors
- Note: Optical sensors are less accurate during movement but work well for still, morning readings
Lower Accuracy:
- Smartphone camera apps (measure via fingertip)
- Accuracy varies widely; not recommended for serious tracking
Recommendation: For daily HRV tracking, a chest strap paired with an HRV app provides the best balance of accuracy and convenience. If using a wrist-based device, ensure it specifically supports RMSSD measurement.
Practical Application: Training and Lifestyle
-
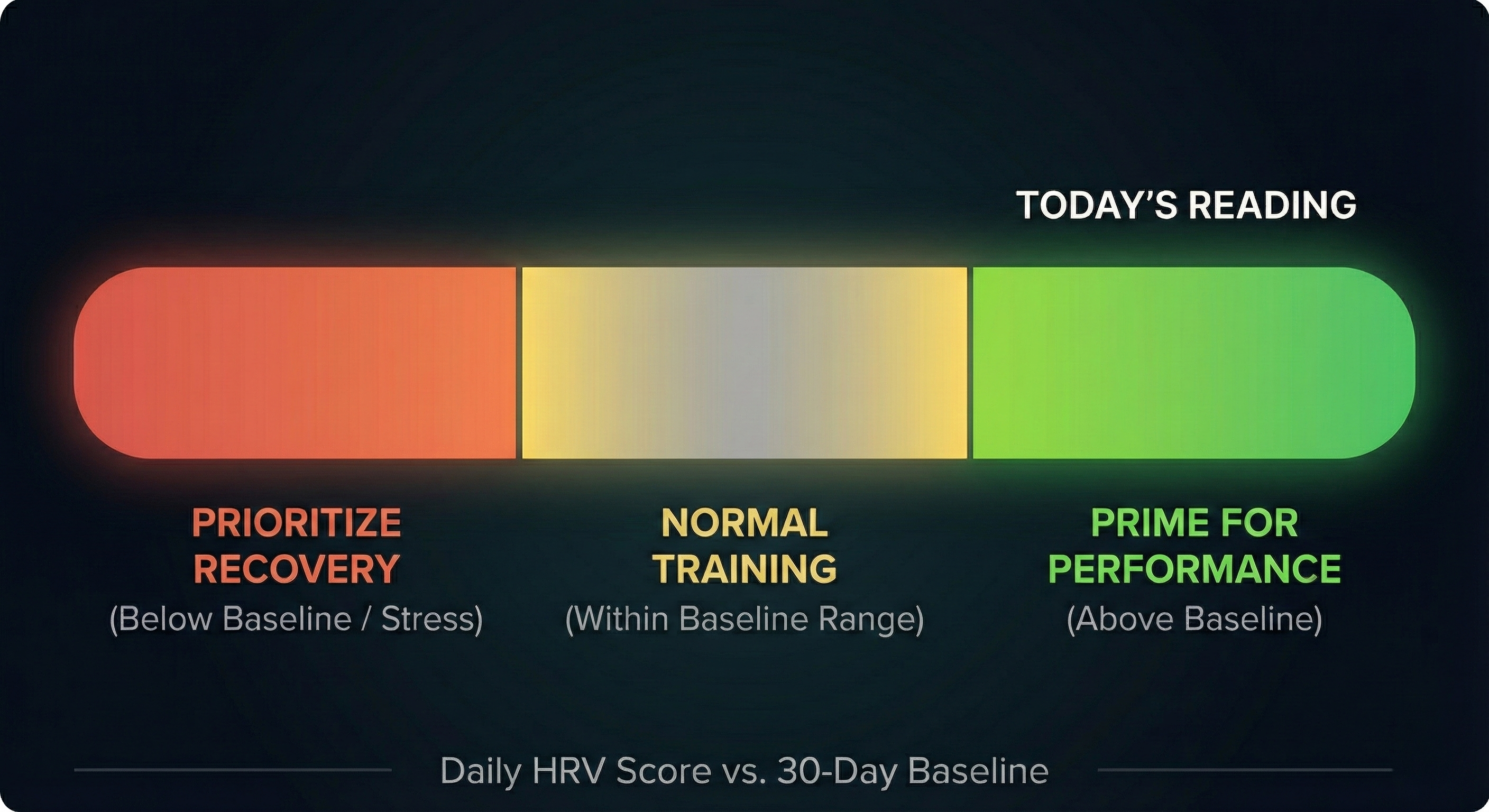
Context is Key There is no universal "good" HRV score. It varies significantly by age and genetics. HRV naturally declines as we get older. Do not compare your score to others. Compare your daily score to your own 30-day baseline (average).
For context only: typical RMSSD values range from 20ms to 200ms depending on age, fitness level, and genetics. Younger, well-trained endurance athletes often have values above 100ms, while older or less active individuals may see values in the 20-50ms range. These numbers are meaningless without your personal baseline—a consistent 30ms is better than an erratic 80ms.
-
Using HRV for Training HRV helps you decide when to train hard, but focus on trends, not single readings.
Single Reading vs. Trends:
- One low reading: Do not panic. It could be measurement error, poor sleep from one night, or normal daily variation.
- 2-3 consecutive low readings: Your body may be telling you something. Consider reducing training intensity.
- 4-7+ days of sustained low readings: Strong signal to prioritize recovery. Reduce volume and intensity, improve sleep, manage stress.
How to Use Your Data:
- Baseline or Higher: Your nervous system is balanced. Your body is ready for high-intensity training.
- Significantly Lower (5-10ms+ below baseline for multiple days): Your sympathetic system is overactive, or your parasympathetic system is suppressed. This suggests unrecovered stress from workouts, poor sleep, or alcohol. It is advisable to prioritize rest or low-intensity movement.
-
Improving Your HRV Research supports several methods to improve autonomic balance:
- Resonance Frequency Breathing: Breathing at a specific slow rate (often around 6 breaths per minute) synchronizes your heart rate with your breath, maximizing HRV.
- Sleep Consistency: Maximizing deep sleep (NREM) promotes parasympathetic dominance.
- Endurance Training: Regular aerobic exercise increases resting vagal tone over the long term.
Timeline for Changes:
- Acute recovery (one night of better sleep): HRV may improve within 1-2 days
- Training load reduction: Expect HRV to normalize within 3-7 days if you were overreaching
- Lifestyle changes (consistent sleep schedule, regular exercise): Noticeable improvements typically appear in 2-4 weeks
- Long-term training adaptations: Building higher baseline HRV through endurance training takes months of consistent effort
What Affects Your HRV?
Understanding what influences your HRV helps you interpret daily changes and make informed decisions about training, recovery, and lifestyle.

Alcohol
Even small amounts of alcohol have a measurable negative impact on HRV. Research shows that a single glass of wine can drop your HRV by an average of 7 milliseconds and increase your resting heart rate by approximately 3 beats per minute. These effects are dose-dependent (more alcohol = greater suppression) and can persist for 24 to 96 hours after consumption. In some athletes, the impact on HRV has been detected up to four days after drinking.
Chronic heavy alcohol use leads to persistently lower HRV and reduced parasympathetic activity.
Sleep Quality and Timing
Poor sleep quality, insufficient sleep duration, and late bedtimes all reduce HRV by suppressing parasympathetic nervous system activity. When you go to bed late or experience circadian misalignment, your body's natural recovery processes are disrupted, which is reflected in lower HRV during and after sleep.
Conversely, consistent, high-quality sleep—especially maximizing deep sleep (NREM stages)—promotes parasympathetic dominance and helps restore HRV to baseline levels.
Exercise Intensity and Recovery
Exercise has a complex, time-dependent relationship with HRV:
- During and immediately after high-intensity exercise: HRV drops sharply due to sympathetic nervous system activation. This is normal and expected.
- Recovery period: After intense training, HRV can remain suppressed for 24 to 72 hours, depending on the intensity of the workout and your training status. Incomplete recovery within this window indicates your body is still under stress.
- Long-term adaptation: Regular aerobic exercise increases resting HRV over time by strengthening vagal tone and parasympathetic capacity. This is beneficial and a sign of improved cardiovascular fitness.
- Overtraining: Excessive training without adequate recovery chronically lowers HRV, signaling that your sympathetic system is overactive and your parasympathetic system is suppressed.
Training Recommendation: Allow at least 24-48 hours between high-intensity sessions if your HRV has not returned to baseline.
Other Common Factors
- Stress (psychological or physical): Chronic stress keeps the sympathetic system activated, lowering HRV.
- Illness: Fighting an infection diverts resources and reduces parasympathetic activity.
- Dehydration: Even mild dehydration can negatively affect autonomic balance.
- Body composition: Higher body mass index (BMI) and increased body fat are associated with lower HRV.
Limitations and Medical Considerations
HRV is a powerful tool, but it is not a complete picture of your health. Understanding its limitations helps you use it appropriately.
When HRV May Not Be Useful
Certain Medical Conditions:
- Arrhythmias (atrial fibrillation, frequent PVCs): HRV calculations assume a normal sinus rhythm. Irregular heartbeats invalidate the data.
- Pacemakers: External heart rate regulation overrides natural autonomic control.
- Certain medications: Beta-blockers, calcium channel blockers, and other cardiac medications can artificially suppress or alter HRV.
Inconsistent Measurement: If you do not measure at the same time, in the same position, under similar conditions, the data is unreliable. Garbage in, garbage out.
When to See a Doctor
HRV is a wellness metric, not a diagnostic tool. Consult a healthcare provider if you experience:
- Persistently very low HRV (below 10-15ms) without explanation: This may indicate severe autonomic dysfunction or underlying health issues.
- Sudden, dramatic drops in HRV (30%+ decline) that do not recover: Especially if accompanied by other symptoms like chest pain, shortness of breath, or extreme fatigue.
- Symptoms that concern you: HRV should complement, not replace, medical evaluation. If something feels wrong, see a doctor—do not rely solely on HRV data.
HRV is One Metric, Not the Whole Story
A complete picture of health and readiness includes:
- Subjective feelings (energy levels, mood, motivation)
- Sleep quality and quantity
- Training load and performance metrics
- Resting heart rate
- Other biomarkers (if available)
HRV is most valuable when used alongside these other signals, not in isolation. Trust your body first, data second.
Appendix: Mathematical Definitions
For those interested in the technical details, here are the standard formulas used to calculate the metrics discussed above.
1. The R-R Interval
This is the raw time duration between two successive R-waves (the peak of the electrical spike) on the ECG.
2. The N-N Interval (Normal-to-Normal)
Raw R-R intervals often contain "noise" or "artifacts." This can include:
- Ectopic Beats: Premature heartbeats that disrupt the rhythm but are not dangerous.
- Motion Artifacts: Sensor movement caused by walking or moving your arm.
- Signal Loss: Poor contact with the skin.
Before calculating HRV, algorithms must "clean" the data. The N-N Interval refers to R-R intervals that have been filtered to remove these artifacts, leaving only the "Normal" sinus beats. All valid HRV calculations use N-N intervals, not raw R-R intervals.
3. RMSSD Formula
RMSSD represents the "Root Mean Square of Successive Differences." It is the primary time-domain measure for estimating parasympathetic tone.
- : The length of a specific interval.
- : The difference in milliseconds between adjacent beats.
- : The total number of intervals measured.
Example Calculation
Let's say your wearable records four consecutive heartbeats with these intervals:
850ms → 900ms → 860ms → 910ms
To calculate RMSSD:
-
Find the differences between adjacent beats:
- 900 - 850 = 50ms
- 860 - 900 = -40ms
- 910 - 860 = 50ms
-
Square each difference:
- (50)² = 2,500
- (-40)² = 1,600
- (50)² = 2,500
-
Average the squared differences:
- (2,500 + 1,600 + 2,500) ÷ 3 = 2,200
-
Take the square root:
- √2,200 ≈ 47ms
This 47ms RMSSD value represents your HRV for this sample. In practice, apps measure hundreds or thousands of beats to get a reliable daily score.
4. SDNN Formula
SDNN is the "Standard Deviation of NN intervals." It reflects the total variability of the system, influenced by both sympathetic and parasympathetic activity.
Note: "NN" refers to Normal-to-Normal intervals (explained in section 2 above)—these are cleaned R-R intervals with artifacts removed.
- : The average (mean) length of all intervals in the recording.
SDNN vs. RMSSD: When to Use Each
RMSSD measures only the differences between consecutive beats, making it sensitive to short-term, rapid changes driven by the Vagus nerve (parasympathetic activity). This makes it ideal for:
- Short recordings (2-5 minute morning readings)
- Tracking daily recovery and readiness
- Monitoring parasympathetic tone
SDNN measures the overall spread of all intervals around the mean, capturing both short-term and long-term variability. This makes it better for:
- Longer recordings (24-hour Holter monitoring)
- Assessing total autonomic balance (both sympathetic and parasympathetic)
- Detecting circadian rhythm patterns and long-term trends
For most consumer wearables and daily HRV tracking, RMSSD is the preferred metric because it can be accurately calculated from brief morning measurements.
References
Cleveland Clinic. (2022). Heart Rate Variability (HRV).
Biopac Systems. RMSSD for HRV Analysis.
Shaffer, F., & Ginsberg, J. P. (2017). An Overview of Heart Rate Variability Metrics and Norms. Frontiers in Public Health.
Cleveland Clinic. Autonomic Nervous System.
Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. (1996). Heart Rate Variability: Standards of Measurement, Physiological Interpretation and Clinical Use. Circulation.
Children's Hospital of The King's Daughters. Sinus Arrhythmia Handout.
Yasuma, F., & Hayano, J. (2004). Respiratory Sinus Arrhythmia: Why Does the Heartbeat Synchronize with Respiratory Rhythm? Chest.
Young, H. A., & Benton, D. (2018). Heart Rate Variability: A Biomarker to Study the Influence of Nutrition on Physiological and Psychological Health? Behavioural Pharmacology.
Boudreau, P., et al. (2013). Circadian Variation of Heart Rate Variability Across Sleep Stages. SLEEP.
Williams, D. P., et al. (2019). Resting Heart Rate Variability Predicted by the Interaction of Inflammation and Sleep Quality.
Welltory. RMSSD and other HRV measurements.
Kubios. HRV Analysis Methods.
TrainingPeaks. HRV-Guided Training.
Oura Ring. Average HRV Across Oura Members.
Kubios. HRV-Guided Training for Endurance Athletes.
Task Force. (1996). Guidelines: Heart Rate Variability Standards.
SpikeAPI. Understanding HRV Metrics: SDNN and RMSSD.